Aria Care Partners, a national provider of dental, vision, hearing, and podiatry care to skilled nursing facilities (SNFs), actively monitors trends in these specialities and in the broader post-acute sector. This report offers an overview of current pathways in ancillary care that are opening new opportunities for better resident outcomes and satisfaction.
Today's SNFs are managing multiple priorities and contending with several headwinds. Although many factors are at play, three stand out for their expected substantial impact on both general and specialty care. These influential forces encompass issue of access, technology, and care delivery (Figure 1).
Medicaid Cuts Impact Access to Care and Skilled Nursing Facility Finances
Current estimates see new eligibilty limits reducing Medicaid budgets by $664 billion over the 2025-2034 period and resulting in 7.6 million fewer Medicaid enrollees.1 SNF exposure to these cuts is substantial, since Medicaid constitutes over 62% of the average facility's payer mix.2
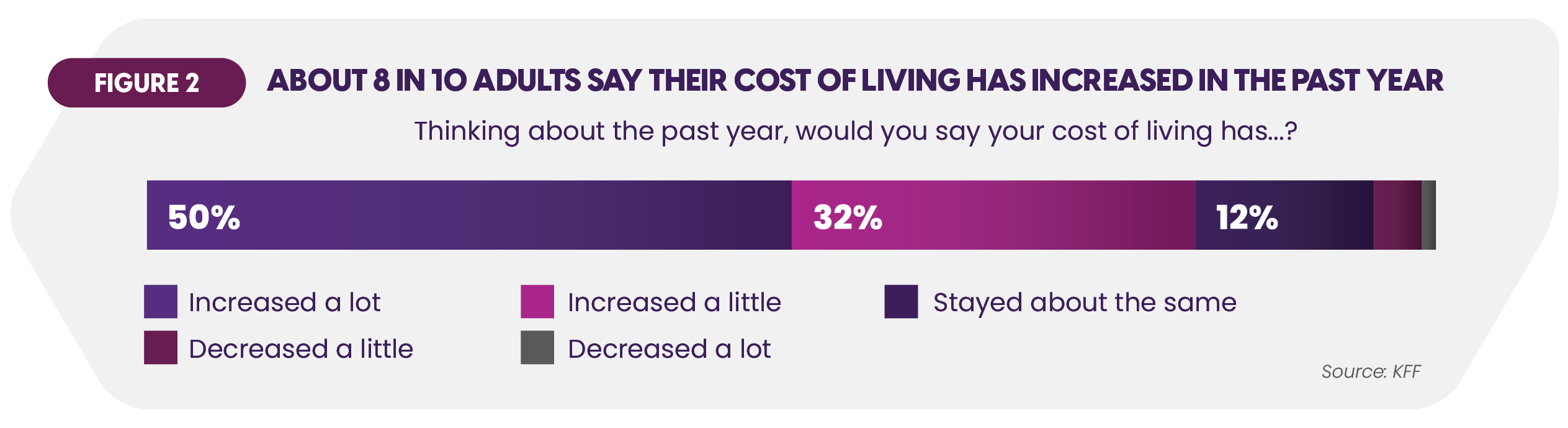
These reimbursement pressures heighten concerns about healthcare access and affordability. Healthcare costs continue to rise. Out-of-pocket spending is projected to increase 3.7% in 2026 to 2027 and 3.9% yearly from 2028 to 2033.3 Medicare Part B premiums have jumped 9.7% in 2026. Such increases are part of a larger picture in which half of Americans worry about rapidly rising overall cost of living (Figure 2).4 In this economic environment, many individuals may defer or avoid care.
From the facility financial side, heavy funding cuts may prompt further consolidation. An analyst report points out that "historically, reimbursement compression has driven structural change in this industry."5
Artificial Intelligence Offers Promising Benefits and Will See Growing Share of Post-Acute Technology Investment
Skilled nursing communities are investing in various technologies. McKnight's annual survey of long-term care providers indicated that 30% are piloting or implementing selected technologies and 27% are implementing multiple systems. However, only 12% regard their technology strategy as mature (Figure 3).6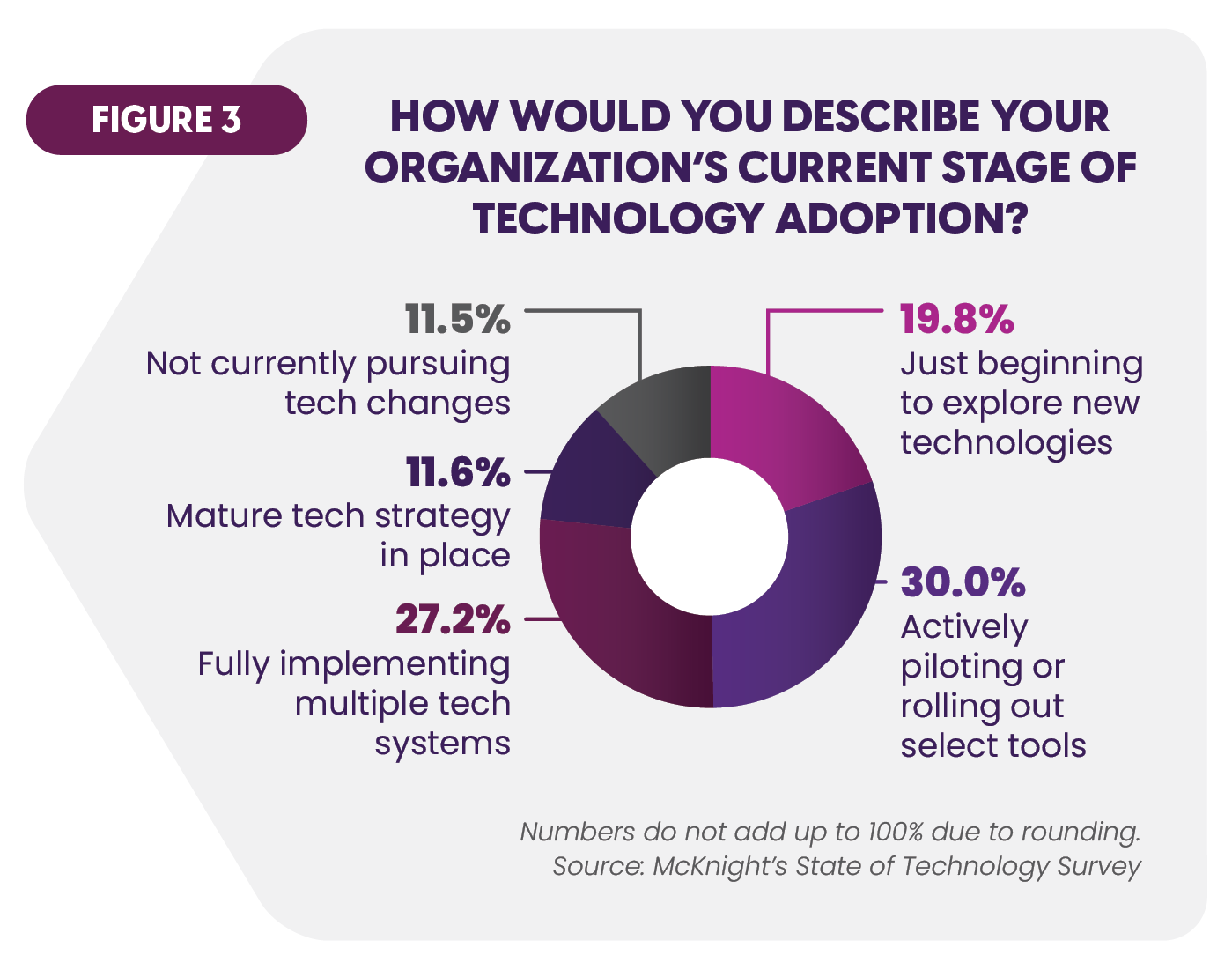
The entire healthcare industry is in heavy pursuit of artificial intelligence (AI) and data analytics technologies that promise significant cost savings, productivity gains, and care quality improvements. In 2025, 22% of healthcare organizations had implmented domain-specific AI tools, a sevenfold increase over 2024.7
Though they tend to have fewer resources than health systems, post-acute organizations are closely watching AI and some are beginning to deploy specific applications. Nursing communities have adopted AI at about half the rate of healthcare organizations overall, but industry observers envision growth as vendors incorporate AI into existing systems used by SNFs.8 AI's share of 2025 private investment dollars flowing to IT companies that target the post-acute sector reached 63%.9
Looking ahead, half of long-term care administrators and a third of nurse leaders see positive or very positive impact from AI over the next twelve months.10 Among the notable emerging uses for AI in SNFs:
- Analytics for powerful insights. For example, "Machine learning models can accurately predict the likelihood of hospitalization or death within the next 7 days among SNF patients. These models do not require additional SNF staff time and may be useful in readmission reduction programs."11
- Fall detection systems will increasingly be powered by AI to gain new levels of sophistication. These systems are projected to grow at 6.2% compound annual rate through 2035.12
- Virtual nursing using real-time monitoring tools that are AI-enabled.13 Many see virtual nursing as a partial solution for healthcare's chronic labor shortages.
Wherever they reside on the adoption curve, SNFs will need to address several issues. One is that residents/consumers are gathering health-related information from generative AI applications. Nearly two million weekly messages are being directed to the ChatGPT bot regarding health insurance questions alone, and 5% of all messages are about healthcare.14 Potential AI errors are another concern. A leading patient safety organization just designated AI as the top healthcare technology risk for 2026.15
Given the accelerating dynamics of AI in healthcare, specific uses will be spotlighted in each of this report's sections on dental, vision, hearing, and podiatry care.
Acuity, Coordination Continue to Pose Substantial Care Challenges
SNFs are grappling with the growing health acuity and multiple chronic conditions among the nation's rapidly expanding aging population. Consider a few data points:
- In 2023, 36% of adults 65 and up had chronic pain that frequently limited activities.16
- By 2035, almost 47% of American adults will be living with obesity.17
- Various geriatric syndromes were seen in more than 90% of hospitalized adults referred to SNFs, with the most-prevalent being falls (39%), incontinence (39%), loss of appetite (37%), and weight loss (33%)."18
- One in nine adults over 65 has Alzheimer's. The risk of developing dementia after age 55 stands now at 42%.19
The complexity of post-acute care places a premium on improving patient transitions between hospitals and SNFs. Better transitions advance the goals of integrated, effective, and value-based care. Noting that 17.4% of inpatient discharges were to SNFs in 2022, a study found that the typical process to be rushed, ill-informed, and disempowering to patients and caregivers. Lack of knowledge is a factor, and the authors conclude that "hospital-based clinicians have a responsibility to understand the different types of post-acute care settings and actively participate in discharge planning."20
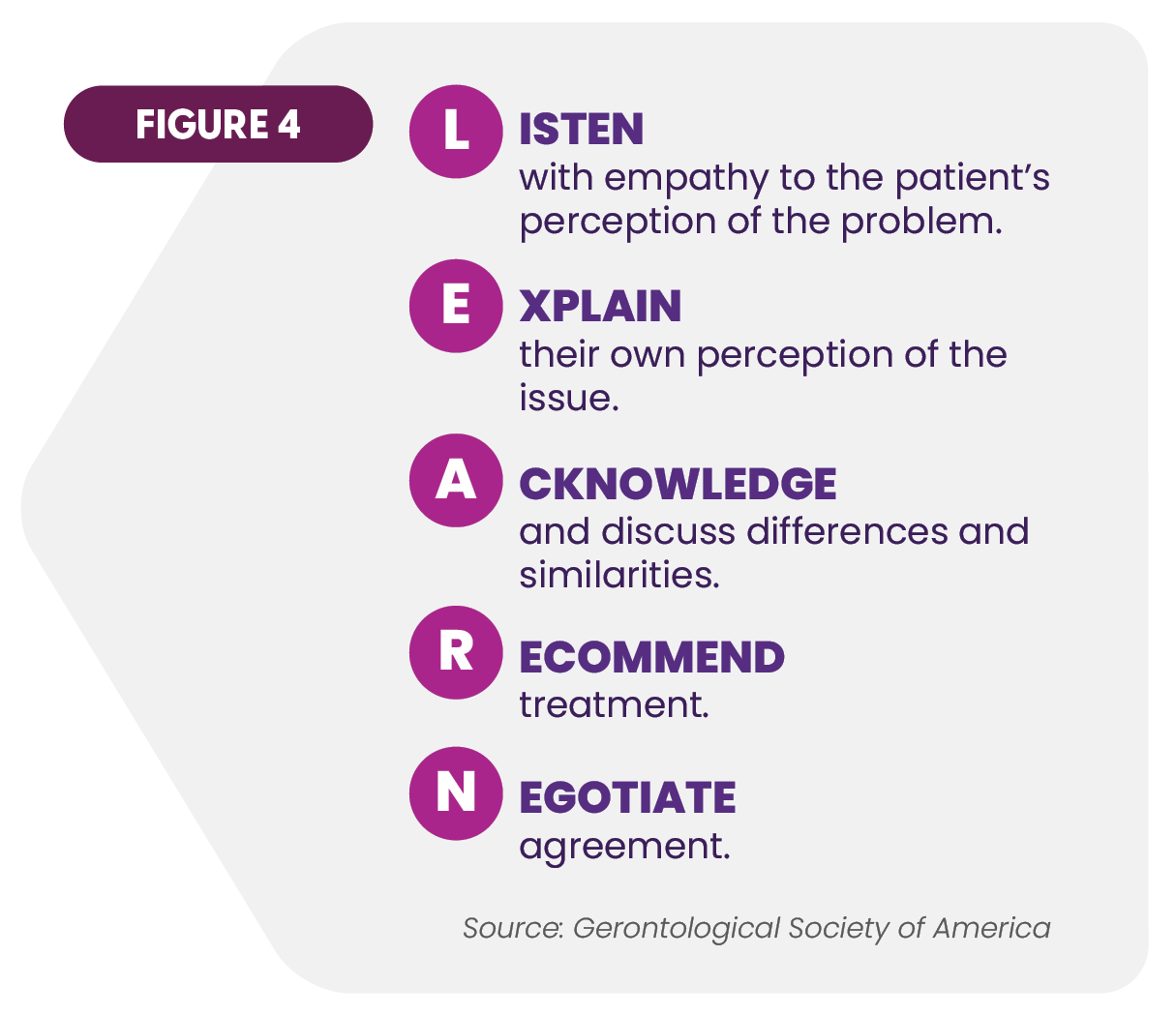
Aria's work confirms the value of improving a related aspect of care delivery. Compassionate, effective communication with older adults is needed to overcome common issues of resistance, understanding, and other factors that can complicate their care. Various strategies have proven effective for caregivers, including the LEARN Model summarized in Figure 4.21
Directions in Four Leading Specialties
Within the skilled nursing ancillary specialties category, dental, vision, hearing, and podiatry care are among the most in demand. As a planning aid for SNF leaders, the following section of this report examines each discipline to convey current directions and themes. Four topics are covered:
- The prevalence and growth of medical conditions.
- Important correlations with other chronic conditions.
- Current themes in care delivery and practice within the specialty.
- Technology developments that are expanding and improving care today and into the future.
Dental - Prevalence of Dental Conditions
Frequently cited statistics quantify the extent of dental problems. From 2017 to 2020, nearly 13% of adults aged 65 and older had untreated decay in one or more permanent teeth.22 Among the same age cohort, 64% had moderate or severe peirodontal disease.23 Self-reported data is also revealing: only 36% of adults rate their oral health as good to excellent.24
Another prevalent condition is missing teeth. Disease causes an average loss of 6.4 teeth in adults over 65.25 Endentulism, the loss of all teeth, occurs in 15% of adults 65 and older, climbing to just under 20% for 75 and older.26 One result is a significant incidence of dentures in post-acute and long-term care settings. A study placed the median edentulism rate at roughly one-third of residents, and observed that chewing efficiency decreases 30% to 40% in complete denture wearers.27 Proper denture fit is thus a major contributor to overall nutrition. 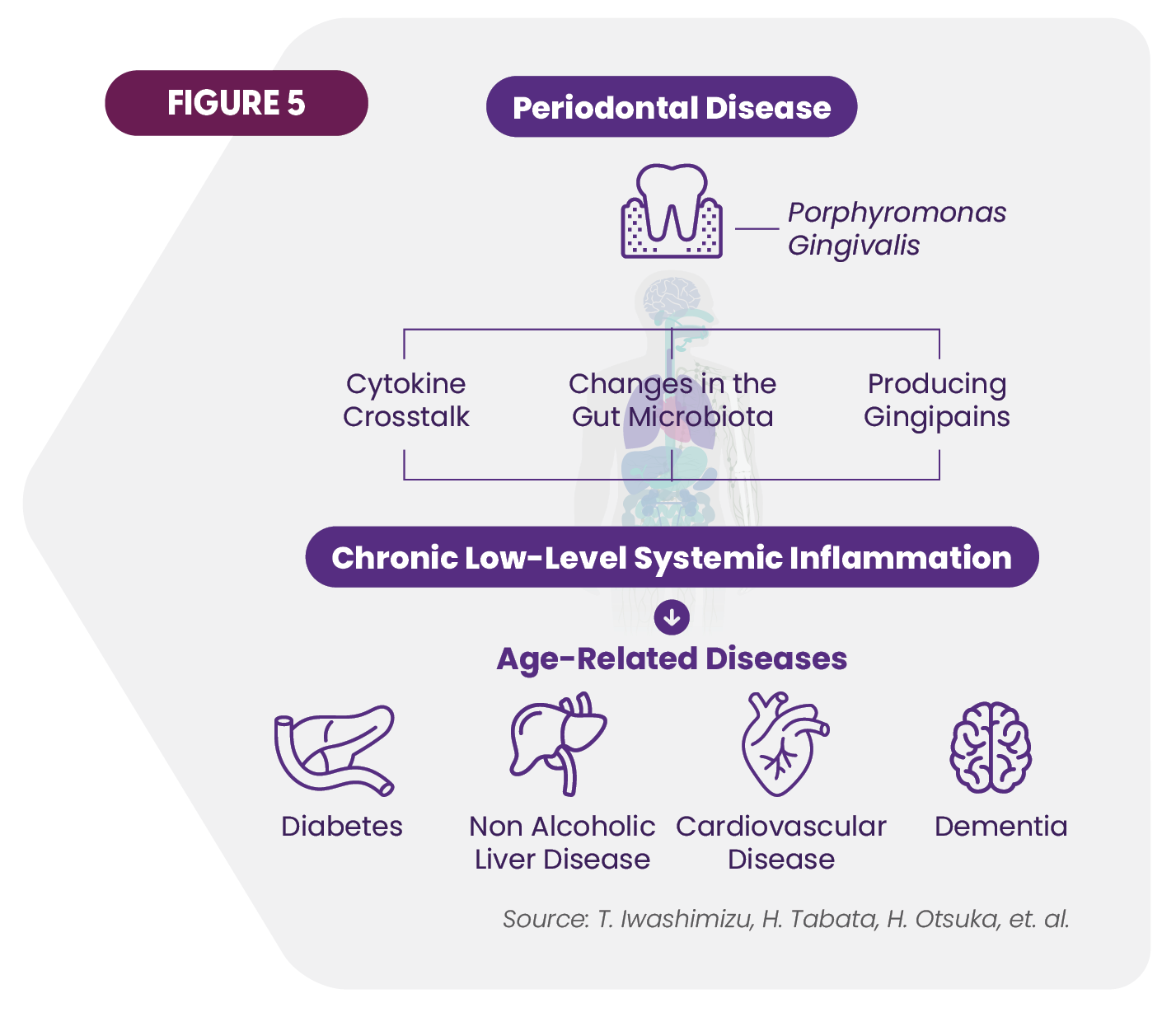
Dental Complications and Correlations
Dental problems have been associated with many chronic and age-related diseases. Scientists have identified several pathways through which periodontal disease creates low-level systemic inflammation that can negatively impact chronic disesase (Figure 5).28
Among the correlations that have been established:
- Type 2 diabetes makes an individual 2.8 times more likely to have severe periodontal diseases and 4.2 time more likely to develop loss of bone that supports teeth.29
- A recent study identified a range of potential downstream consequences of insufficient denture hygiene, such as denture-related somatitis, systemic fungal infections, malnutrition, and aspiration pneumonia.30
- Depression and oral problems show correlations. Various findings have concluded that over half of adults with moderate depression have periodontal diseases, and more than one-third have untreated dental decay.31
Well under half of adults are aware of the dental connections with potentially harmful chronic conditions (Figure 6).32

Dental Care Delivery Issues
A dental executive summarizes a prevailing delivery issue in noting that "there is a common misperception that dentistry is elective...and only necessary when there is pain."33 Promoting preventative care is vital, especially for diabetics.34
Dental anxiety deters many people from seeking regular care. A 2024 survey found widespread dental fear, with 45.8% reporting moderate fear and 26.8% reporting severe.35 Twenty-one percent of adults have avoided dental care due to anxiety.36
The fear factor underscores the value of onsite visits by dentists with experience and understanding of the SNF population. "Emotional Intelligence is a cornerstone of effective patient-dentist relationships," states a recent analysis. "By fostering trust, improving communication, and managing emotional challenges, dentists can enhance the quality of care and patient experiences."37
Another delivery consideration is ensuring broad access to dental care. Insurance gaps pose access barriers: 26% of surveyed individuals have no insurance, and only two-thirds of adults over 60 say they are insured (Figure 7).38
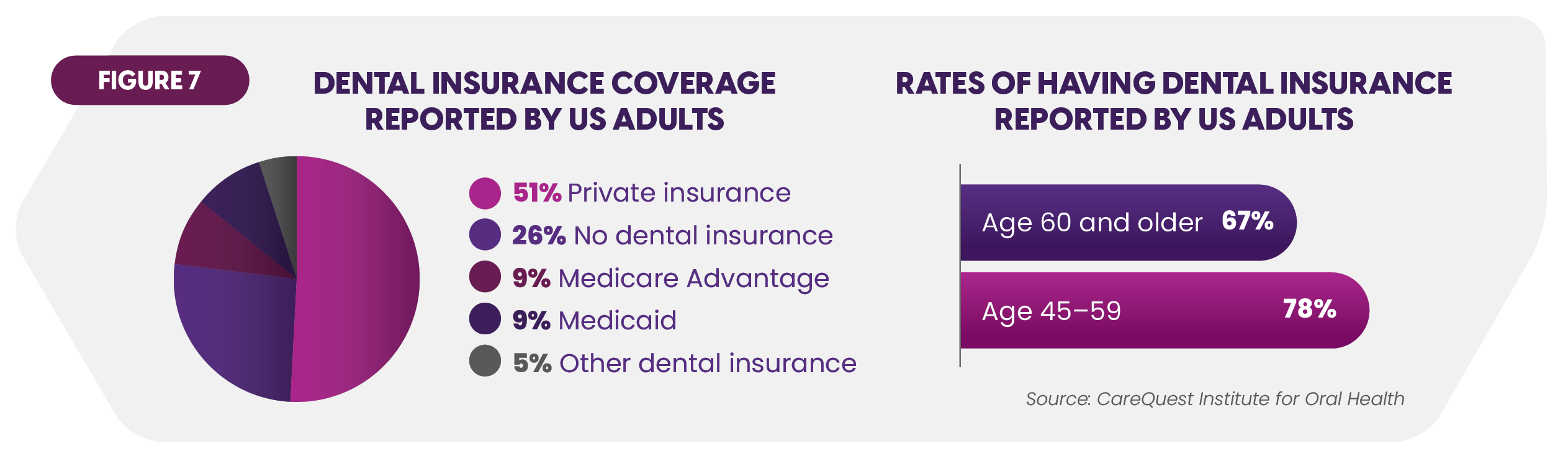
Socioeconomic obstacles are also gaining attention. A government report states that "recognizable oral health disparities and inequities" exist among populations with limited economic resources and poor access to dental care.39 The likelihood of black adults having tooth issues is 67% greater than for white adults.40 SNF communities are attuned to these factors since many exclusively treat the underserved.
One strategy to overcome the access problem is mobile dental clinics, an expanding market anticipated to be $2 billion by 2033.41 Aria's onsite service is a proactive form bringing mobile dentistry to individuals at their current location.
Dental Technology Trends
- AI is playing a prominent role as dentistry continues to go digital. The growth trajectory for dental AI between 2025 and 2034 is almost 22% compounded annually to reach $3.2 billion.42 Examples of promising applications include:
- Radiography. Enhanced imaging for earlier, more precise diagnosis of cavities, bone loss, and other issues and risks.
- Implants. Assists surgical planning and implant placement. AI can also drive robotics-based surgical procedures.
- Patient engagement.Tools are being developed to help individuals understand oral health, guide them on personal risk factors, and issue alerts for dental visits.
- Documentation. Ambient AI permits dentists to speak naturally during an exam and have the software automatically build a structured note from the conversation for review by the dentist.
- Smart toothbrushes. Users receive AI-driven feedback on pressure, time taken for brushing, and overall brushing performance. Chemical microrobots are being developed that can recognize and automatically remove biofilm from teeth.43
- 3D Printing. Aria uses 3D printing in its provision of dentures to SNF residents. This technology is expanding globally at over 21% through 2032.44 Coupling design software with a convenient "printer" that outputs layers of material enables personalized, best-fit dentures from a person's impressions and molds.
- Digital Smile Design uitlizes software, photos, and videos, to generate virtual images of a patient's smile, allowing dentists to design the intended appearance at high precision. Sensors can track jaw movement for heightened accuracy.
- Dental Lasers are used for everything from treating cavities to tissue removal to faster teeth whitening. This fast-growing market will reach $754 million by 2034.45
- Virtual/Augmented Reality. Some are experimenting with this technology to help patients visualize and understand procedures and reduce anxiety. Digital images can be merged with real images and virtual actions can be realistically displayed. A poll of people with dental fear saw 71% indicating interest in some form of digital treatment for their anxiety.46
Vision - Prevalence of Vision Problems
Corrected vision that measures 20/40 or worse is generally defined as impaired, and the rate among adults over 70 has been pegged at almost 28%.47 Significant vision loss is reported by 6.3% of Americans age 65-74, 7.4% for 75-79, and 9.8% at 80+.48 About 16% of those between 75 and 84 cannot read newsprint even with corrective lenses, jumping to 27% for individuals 85 and older.49 Impairment and blindness are projected to double worldwide over the next 30 years.50
Seniors tend to experience four major eye issues that can impair vision: glaucoma, macular degeneration, diabetic retinopathy, and cataracts. Age-related macular degeneration affects approximately 20 million Americans.51
Vision Complications and Correlations
Vision Problems are correlated with-and can exacerbate-a number of other serious ailments:
- Diabetes. Diabetics exhibit two to five times greater likelihood of developing cataracts.52 Diabetic retinopathy has been calculated to occur among 26% of diabetics.53
- Falls. A study of Medicare beneficiaries with self-reported vision impairment found significantly higher fall occurrence, fear of falling, and activity limitations due to those fears.54
- Mental and Social Impacts. A number of studies have linked vision loss to depression. One put the likelihood of depression 1.6 to 2.8 times compared to those without vision impairment.55
- Cardiovascular Disease. Approximately 1 in 4 adults with vision impairment reported a cardiovascular disease diagnosis versus 1 in 10 respondents without impairment.56
- Hearing Loss. About 33% of adults over 65 with vision loss also suffer hearing impairment, as opposed to 14% for those without vision loss.57
Vision Care Delivery Issues
The vision care products and services market is large and expanding, expected to attain $71.5 billion by 2035.58 Yet many individuals have had limited eye care. A study of over 1,000 participants found that 55% had not undergone an exam in two or more years.59 Primary reasons cited for avoidance were lack of insurance (28%), no perceived eye problem (22%), and cost (16%). Even among adults at high risk, 4 in 10 forgo annual eye checks.60
Vision professionals are increasingly attentive to the need to counteract the effects of looking at digital screens. Between television viewing and growing use of digital devices, older adults are estimated to be spending 4 to 5 hours per day engaged in screen-based activities and my be joining the 65% of Americans who are said to experience various forms of digital eye strain from such usuage.61
Eye care is also facing a decline in supply of medical professionals. A study claimed that "opthalmology" is one of the medical specialities with the lowest rate of projected workforce adequacy by 2035.62 Optometrists are viewed as part of the solutions, since the profession counts 48,000 doctors with steady annual growth of one percent.63
Vision Technology Trends
- AI. AI is making major inroads in vision care. A significant application is AI based screening. Autonomous diabetic retinopathy screeners are showing strong capabilities in identification of sight-threatening disease, and experts see AI being deployed in routine diabetic eye checks to bolster prevention of vision loss.64 Another example involves the combination of image recognition technology with AI to create smartphone apps that can deliver verbal narration of what is occurring around a visually impaired individual.65
- Portability. Technology is driving greater equipment portability to assist mobile caregivers by reducing physical size and expanding features. An example is a portable retinal camera with intelligent diagnostic screening tools for detection of diabetic retinopathy (Figure 8).
- Smart glasses. Intelligent glasses continue to add power and sophistication to support the visually impaired. Figure 9 shows a model that includes vision-enhancing features such as high-definition screens, auto focus, and state-of-the-art-cameras.
- Imaging. Optical Coherence Tomography (OCT) enables visualization of the retina and optic nerve at very high resolution for early detection of glaucoma or age-related
 macular degeneration. The OCT market is growing at a rapid 10% annual clip to reach $4.8 billion in 2034.66 AI is also being embedded in OCT devices.
macular degeneration. The OCT market is growing at a rapid 10% annual clip to reach $4.8 billion in 2034.66 AI is also being embedded in OCT devices. - Implants. A system called photovoltaic retina implant microarray (PRIMA) directs near-infrared light to an implant to counter central retinal atrophy and restore sight.67
Hearing - Prevalence of Hearing Loss and Problems
The hearing loss statistics are remarkable. The rates for U.S. adults are 13% for ages 40-49, 68% for 70-79, and 90% for 80 and above.68 Hearing loss is said to double during every decade of life from the second to the seventh.69 Tinnitus is viewed as a major problem by 120 million people worldwide, largely over age 65.70
As with vision, hearing issues are not monolithic. Professionals check for a range of problems in three categories:
- Sensorineural hearing loss - damage to the inner ear or hearing nerve often caused by aging and illness.
- Conductive hearing loss - sounds not reaching the inner ear due to infections, blockages, and structural issues.
- Mixed hearing loss - a combination of the first two.71
Hearing Complications and Correlations
Hearing loss interacts with a diverse set of health conditions. Among the most prominent and consequential:
- Dementia and mental health. Roughly 40% of older adults with dementia report difficulty hearing.72 Midlife peripheral hearing loss has been causally associated with 9% dementia cases.73 AARP recently named hearing loss a leading risk factor for dementia.74
- Social isolation. Hearing difficulties often deter people from participating in social activities. One study revealed that the hearing impaired exhibited a "significantly smaller" social network size with fewer non-kin members relative to a control group.75
- Cardiovascular disease. Researchers believe that cardiovascular disease can reduce blood flow to the ear, triggering damage to different parts of the auditory system.
- Diabetes. A meta-analysis of studies encompassing some 4,000 diabetics and an equal number of control subjects indicated that individuals with Type 2 diabetes had a 4.19 times higher risk of hearing loss.76
- Parkinson's disease. A recently published review showed that people with Parkinson's disease were 1.82 times more likely to have hearing loss than those with no disease, adjusting for age factors. Hearing loss "may represent an early non-motor symptom."77
Hearing Care Delivery Issues
Aria providers often encounter SNF residents who have had minimal previous hearing care. Reluctance to seek care is common. The average time between a person noticing the onset of hearing loss and discussing it with a medical professional is about 4.5 years.78 A third of adults over 50 are said to be secretive about their hearing out of fear of being judged.79
Hearing aids are central to efforts to mitigate hearing loss. Use is substantial and growing (Figure 10).80 Unfortunately, costs that can run several thousand dollars discourage adoption for many. Fifty-six percent of survey respondents say hearing aids are too expensive.81
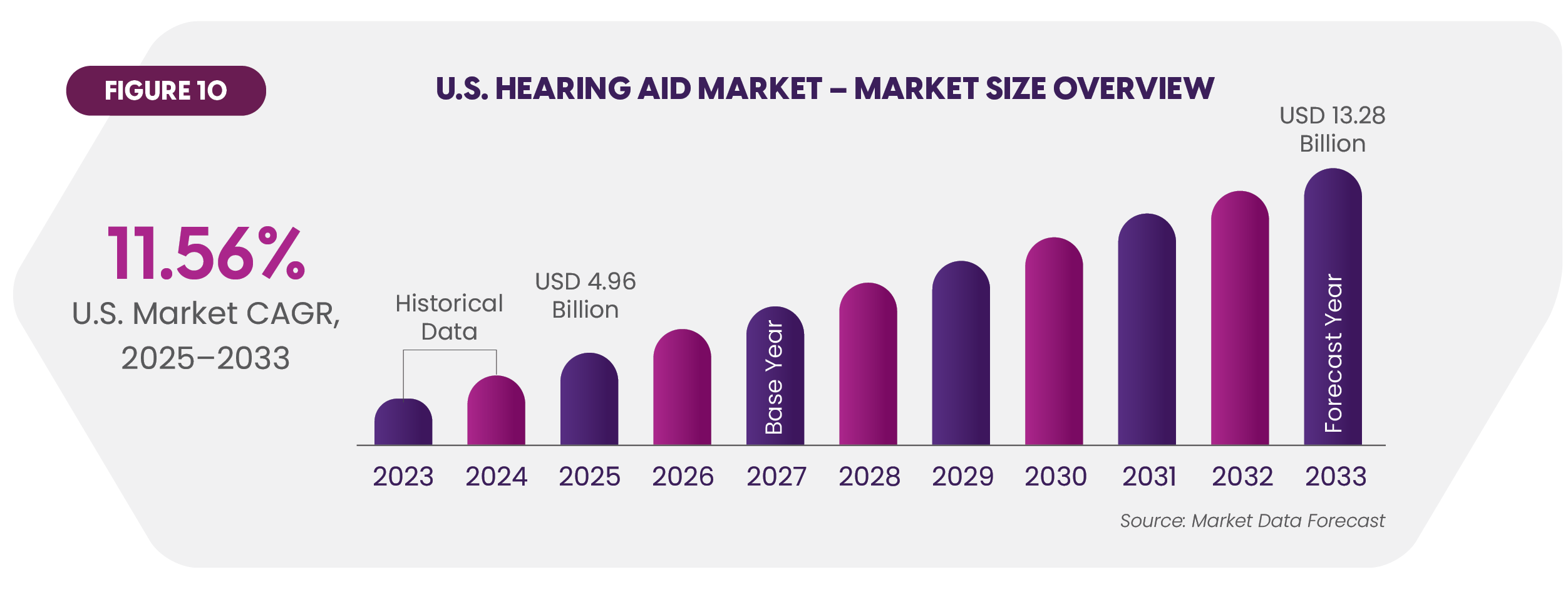
Insurance is therefore always a critical factor. An analysis showed that 28% would purchase hearing aids if insurance covered $500, 36% if $1,000, and 54% if total coverage.82 Aria Care Partners has long recognized this need and offers hearing policies for residents it serves. It should be noted that while most Medicare Advantage plans carry hearing benefits, significant coverage variability exists.
Hearing Technology Trends
- AI. AI and machine learning are becoming driving forces in enhancing hearing. A recent review described two transformative AI uses.83 One is "real-time environmental adaptation" whereby hearing aids "can tell the difference between sounds" and make automatic adjustments to boost hearing such as "muting wind noise" or "lowering background chatter." Another is "personalized hearing." Machine learning tracks user adjustments and preferences and begins to make them automatically. "The more you use them, the better they get," notes the author.
- Digital hearing aids. Digital aids continue to gain adoption as they take increasing advantage of Bluetooth, smartphones, noise cancelling, and other technologies. The market will be $15 billion by 2030.84 They are participating in the broader trend to smart wearable devices and are being linked with other wearable tools like language translation, fall detection, and fitness tracking. Hearing aids build into smart glasses is an emerging development. These glasses aim to overcome the perceived negatives of in-ear aids. (Figure 11).
- Sensor support. Sensors are playing a leading role in the various advanced digital hearing solutions. Integrated with hearing aids, they provide sophisticated monitoring and capturing of data on a wide range of individual and environmental auditory variables.
Podiatry - Prevalence of Foot and Ankle Problems
SNF residents are likely to present on admission with at least one foot or ankle disorder. Pain is common, and it can emanate from multiple locations on the foot's complex structure (Figure 12).85
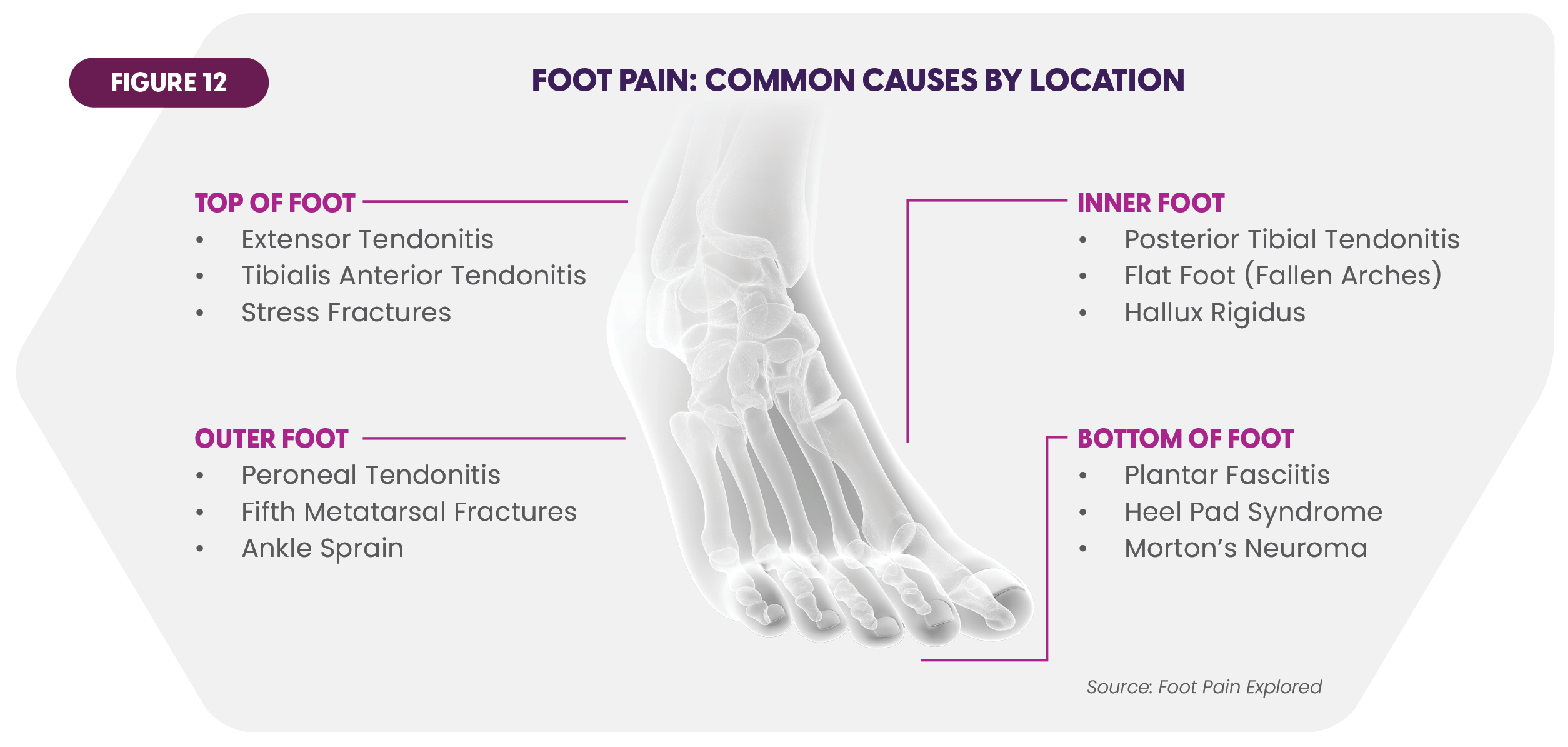
Eight in ten Americans report experiencing foot pain at some point in their lives, with 39% classifying the pain as severely limiting.86 Serious conditions such as Peripheral Arterial Disease (PAD) are also prevalent. PAD constricts blood flow to the legs and can cause ulcers. It afflicts over 21 million Americans.87
Podiatry Complications and Correlations
SNF podiatry care must be alert to important linkages with foot problems:
- Falls. Over 25% of older adults report falling each year.88 Foot pain and disorders constrain mobility and pose a clear fall risk. Studies of podiatry interventions such as assessments, proper footwear, and targeted exercises show significant reductions in the frequency of falls.89
- Diabetic foot problems. Diabetes is correlated with nerve damage, foot ulcers, vascular disease, and a greater potential for lower extremity amputation. The lifetime risk of developing a diabetic foot ulcer has been calculated at between 19% and 34%, and recurrence after initial healing reaches 65% within 5 years.90
- General frailty. The prevalence of foot problems increases significantly as frailty worsens: 95% in the frail versus 63% in the non-frail.91
- Mental Health. A review of multiple studies concluded that "negative emotional and cognitive factors were more common in people with foot/ankle pain compared to those without foot/ankle pain."92
Podiatry Care Delivery Issues
It is likely that many admitted non-diabetic SNF residents have had little exposure to professional podiatric care. Overall, just 32% of adults with foot pain received a formal diagnosis in 2025.93 Even among diabetics, only 54% of participants in a survey acknowledged the importance of daily foot inspections, and 27% actually consulted a professional.94 "Enhancing foot care knowledge and practices among diabetes patients is vital to reducing the burden of dieabetic foot complications," conclude the survey authors.
Self-care, particularly among the elderly, is another challenge. Interviewed older adults cite hurdles such as uncertainty on where to obtain advice, difficulty finding appropriate self-care products, reluctance to ask family members for help, lack of motivation or patience for care, and other reasons.95
Improper footwear is a key variable in the care equation. Podiatry professionals provide recommendations for footwear that minimizes pain and deters falls (Figure 13).

Podiatry Technology Trends
- AI. AI tools can peform advanced gait analysis from video and sensor data, examining the information alongside relevant patient history. The aim is earlier and more precise detection of abnormalities. AI is also helping generate predictive models that clinicians can use to anticipate complications such as diabetic ulcers.
- Smart footwear encompasses intelligent insoles, socks, and shoes that incorporate sensor and Bluetooth technologies. Intelligent shoes have been designed to monitor diabetic foot ulcers, track rehabilitation progress, and detect falls among older people.96 Potential enhancements include adding GPS tracking, obstacle detection, and other applications.
- 3D Scanning and printing is creating rapid, cost-effective, highly personalized custom orthotics. U.S. 3D printing for prosthetics is expanding 7.5% annually through 2034 when the market will attain a level of $1.2 billion.97
- Treatment innovations. Medical technology is producing exciting clinical developments in the podiatry realm such as:
- Cartilage regeneration. To counteract age-related degeneration of joint strength, new techniques are using advanced materials to hold the patient's own stem cells in place until new cartilage forms.98
- Swift Microwave Therapy. This FDA-approved technology targets plantar warts using isolated microwave radiation.
- Virtual Reality. Virtual reality's impressive and interactive experiences can help patients understand and cope with foot pain and promote adherence to therapies.
Conclusion
The data paints a clear picture for skilled nursing facilities. The extent of problems, relationships with chronic conditions, and advancements in technology and care delivery make dental, vision, hearing, and podiatric services an increasing priority. Those specialities are also intertwined with major, urgent industry forces exerted by developments in access, AI and related technologies, and growing patient acuity. Successful navigation of this landscape involves a commitment to compassionate, comprehensive, convenient ancillary care. Aria Care Partners will continue to support SNF communities through ongoing surveillance of market and clinical directions and ancillary care programs aligned with today's priorities and the evolving needs of tomorrow.
 Home Page
Home Page Home Page
Home Page

 Share to Twitter
Share to Twitter
 Share to Linked In
Share to Linked In

